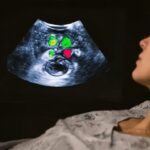
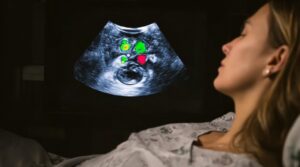
Primary care gives women a central place to receive preventive services, reproductive care, chronic disease treatment, mental health support, and referrals for specialized treatment.
Access to consistent primary care improves health outcomes across many stages of life, including adolescence, pregnancy, postpartum recovery, and older adulthood.
Women often rely on primary care providers for routine screenings, contraception counseling, treatment for common illnesses, and support for long-term conditions such as diabetes or hypertension.
Improved access transforms the primary care visit into a broader conversation about physical health, reproductive needs, mental health, and social concerns.
More comprehensive visits give women stronger relationships with providers and greater opportunities to prevent health problems before they become emergencies.
Barriers Women Face in Primary Care

Women face several obstacles when trying to access primary care services. Limited appointment availability often forces patients to wait weeks or months for routine visits.
Long delays can discourage preventive care and increase reliance on urgent care centers or emergency rooms. Financial concerns also create major barriers.
Insurance gaps, high deductibles, and out-of-pocket costs may prevent women from seeking treatment until symptoms worsen.
Transportation problems and childcare responsibilities create additional challenges. Many women balance work, caregiving, and household duties while attempting to schedule medical appointments during standard business hours.
Fragmented health care systems create another problem. Women commonly receive reproductive services through OB-GYN providers while chronic disease management and preventive screenings occur in separate primary care settings. Mental health treatment may involve different clinics or providers. Multiple systems can lead to communication problems, repeated testing, inconsistent treatment plans, and gaps in follow-up care. Structural barriers also affect women differently depending on socioeconomic status, race, ethnicity, and geographic location. Rural communities often have fewer providers and longer travel distances for appointments. Lower-income women may have reduced access to newer technologies and digital health tools. Some modern care models and telehealth services only reach narrow groups of consumers, leaving underserved populations with fewer options. Improved access changes primary care visits by creating earlier, more complete, and more patient-centered interactions. Easier appointment scheduling, reminder systems, telehealth visits, and expanded clinic hours help women seek care before medical concerns become severe. Earlier treatment often leads to better outcomes and reduces the need for emergency services. Improved access changes primary care for women by creating earlier, more complete, and more patient-centered interactions. Easier appointment scheduling, reminder systems, telehealth visits, and expanded clinic hours help women seek care before medical concerns become severe. Patient-centered communication becomes more possible when visits are not rushed or delayed for long periods. Providers can begin appointments with open-ended questions such as, “What would you like to talk about today?” or “Would you like to become pregnant in the next year?” Questions like these encourage trust and allow women to discuss concerns that may otherwise stay unspoken. More accessible visits also create opportunities to address several health needs during one appointment. Areas commonly discussed during improved primary care visits include: Broader discussions can improve early detection of health problems and increase patient satisfaction. Evidence supports the value of integrated women’s health services in primary care settings. One study reviewed 666 patient charts, including 314 before implementation of a primary care-based women’s health clinic and 352 after implementation. Findings suggest that better access and integrated care improve communication about reproductive and sexual health. Digital health tools can further improve patient care. Nearly 90% of primary care providers in one study viewed digital health adoption as useful for improving care quality. Telehealth visits, electronic reminders, patient portals, and online scheduling systems can reduce barriers related to transportation, work schedules, and clinic availability. Strong primary care systems connect physical health, reproductive care, behavioral health treatment, and social support services. Integrated care allows providers to address many patient concerns within one coordinated system instead of separating treatment into disconnected clinics. Team-based care models improve coordination among providers. Care teams may include: Collaboration among providers improves communication and creates more consistent treatment plans. Integrated primary care systems can coordinate specialty referrals, behavioral health treatment, nutritional counseling, and social support programs. Women with chronic illnesses, pregnancy-related concerns, or mental health conditions may benefit greatly when providers communicate closely with one another. More comprehensive primary care can also reduce unnecessary specialist referrals. One study examining a women’s health clinic integrated into primary care found that gynecology referrals decreased from 18% to 11% after implementation. Results suggest that more women’s health concerns were successfully managed inside primary care settings. Sharp declines in structured medical support during the postpartum period can create serious risks for physical and mental health. New mothers often manage multiple responsibilities while recovering physically and caring for newborn children. Insurance changes, scheduling difficulties, transportation problems, and childcare demands can make follow-up appointments difficult. Researchers have described this situation as a postpartum cliff because patients experience a sudden reduction in organized support after delivery. Better access to primary care during postpartum recovery can reduce complications and improve continuity of care. One study examined 353 pregnant or recently postpartum patients receiving treatment at a large academic medical center. Half of the participants received an intervention that automatically scheduled primary care visits during the first four months after childbirth and sent tailored reminders and messages encouraging follow-up care. Findings suggest that improved scheduling systems, reminders, and stronger primary care connections can reduce avoidable emergency care use after childbirth. Better postpartum access also supports mental health treatment. Depression and anxiety frequently affect women after delivery, yet many patients struggle to receive timely support. Primary care visits create opportunities for screening, counseling referrals, and medication management during a critical period of recovery. Improved access changes primary care visits by making them more preventive, coordinated, and patient-centered. Easier scheduling, telehealth services, reminder systems, and expanded clinic hours allow women to receive treatment earlier and discuss more concerns during one appointment. Comprehensive primary care systems allow providers to address preventive screenings, reproductive health, chronic illnesses, mental health concerns, and social needs in coordinated settings. Integrated care models also improve communication among providers and reduce unnecessary referrals.
How Better Access Changes the Visit
More Comprehensive and Coordinated Care

Postpartum Care as an Example
Postpartum care demonstrates how improved access can significantly affect women’s health outcomes. Many women lose regular contact with health care systems after childbirth.
Summary
Related Posts: